Hip Preservation Surgery Relieves 20 Years of Pain
A 37-year-old man presented at Duke with persistent hip pain from a high school injury that occurred at age 17. The pain was sharp and worsened with hip flexing and prolonged sitting. The patient enjoyed intense exercise, but physical activity worsened his pain and he was unable to participate at the level he desired.
Tally Lassiter Jr, MD, MHA, a Duke sports medicine orthopaedic surgeon, consulted with the patient and observed the following from physical examination and test results:
- Antalgic gait
- Limited motion
- Positive Trendelenburg sign
- Positive Stinchfield test
- Positive flexion, adduction, and internal rotation (FADIR) sign and positive flexion, abduction, and external rotation (FABER) sign
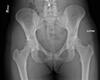
Radiography showed the following:
- Alpha angle of 80°
- Head-neck offset of 0°
- Positive crossover sign
Question: As a result of these findings, what two conditions did Lassiter suspect were the sources of the patient’s pain?
Answer: Femoroacetabular impingement (FAI) and an anterior-superior labral tear, both of which were confirmed by results from magnetic resonance arthrography.
Lassiter performed arthroscopic acetabuloplasty and femoroplasty to remove the hip impingement, labral repair with three knotless suture anchors, and a cam lesion excision to correct the alpha angle. The interportal capsulotomy was not closed.
A relatively new procedure, hip arthroscopy with acetabuloplasty and femoroplasty can increase the longevity of the native hip, prevent early arthritis, and help avoid or delay the need for hip replacement in patients with FAI.
Lassiter notes that there are certain patient populations who generally have the best outcomes from the procedure: young athletes, such as soccer and hockey players, and people in their mid- to late-30s who develop symptoms from old injuries and want to return to their active lifestyles, such as the patient in this case.
But, he cautions, it is not always the best approach for young patients with hyperflexible hip joints and dysplasia (shallow sockets), such as cheerleaders and gymnasts. “In these cases, the shallow acetabulum can be made unstable with the procedure, so we have to be extra cautious with treatment. It’s also not the best option for patients in their 40s and 50s who have early advanced arthritis from FAI.”
Lassiter notes that Duke’s hip preservation expertise encompasses arthroscopic surgical repairs for patients with torn hamstring tendons and those with gluteal pain syndrome (hip bursitis), who may have actually torn a tendon, if corticosteroid injections do not relieve pain. Beyond arthroscopic procedures, many complex surgeries are available to help prevent patients from developing arthritis and requiring hip replacements at a young age.
“If a young, active person is considering hip replacement surgery, it would be wise for them to consult with an orthopaedic surgeon who specializes in hip preservation to determine whether there are other options,” says Lassiter. “We know that hip replacements often wear out in about 15 years, so we try to avoid that in young people if at all possible.”
This patient was discharged home following the outpatient surgery and started physical therapy, using a continuous passive motion machine and a cold therapy device. “He reported that his pain was dramatically better than it was before, even the first day after surgery,” says Lassiter.