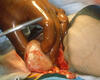
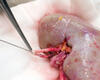
The Duke adult kidney transplant program’s one-year conditional survival rate rose to 99.69%--exceeding the national average by two percentage points, according to data from the Scientific Registry of Transplant Recipients (SRTR).
The 2021 data highlights the program’s rank in the top one percent for both outcomes and quality, says Matthew J. Ellis, MD, medical director of the adult transplant program.
“These rankings reflect well on the U.S. transplant community in general,” Ellis says. “An overall conditional survival rate of about 97% indicates broad success. Exceeding 99% is an achievement we are very proud of.”
Ellis noted that the report’s outcome data is particularly significant because Duke is among the top 25% in total kidney transplant volume. “As a program, you focus on outcomes and quality, of course, but it’s exciting to be successful in outcomes when we perform a relatively high number of procedures.” During the past three years, the kidney transplant program has completed approximately 200 procedures annually.
The conditional survival and outcomes rankings are particularly significant, Ellis says, because of the program’s history of accepting patients with challenging comorbidities who are turned down elsewhere, including HIV, sickle cell, cardiomyopathies, and high BMI (up to 40).
“We appropriately push the envelope in trying to help patients receive a transplant when they are turned down at other centers,” Ellis says. “But we are also honest with patients and families about the risks involved and what we can and cannot do.”

Duke offers comprehensive evaluation and care to your patients with kidney disease. Our experienced team works with you and other Duke specialists to diagnose and manage kidney disease and related care needs.
Prioritizing the organ match
Matching kidney to patient and ensuring organ health are priorities that contribute to Duke’s successful outcomes, Ellis says. Organ assessment is based on a kidney donor profile index that incorporates donor age and health, creatinine levels, as well as cold time before transplant. In some cases, the team requests a biopsy and engages nephropathologists to determine the histological health of the organ. Specialized management of organs before transplant is another key factor in outcome quality.
Duke now accepts nearly one-quarter of organs from living donors, reducing the need for deceased donations, which are more challenging to transport and use. The program also emphasizes early referral options for preemptive transplant. By assessing organ health earlier in the referral process, some patients receive transplants more quickly.
The SRTR rankings, Ellis says, reflect the effectiveness of the adult transplant team. “We have a good program because we have great people working together toward a single goal,” Ellis says. “Duke has all the parts of the puzzle—coordinators, clinicians, physicians, administrators—and these people care a great deal about their work. That level of focus and collaboration translates into exceptional outcomes.”
Better outcomes mean more patients are eligible for transplant. “A patient with diabetes who has experienced a heart attack was considered a very complex patient 10 or 15 years ago. But that patient profile is not unusual in our program today, and we work with patients who have even more complications,” Ellis says.