Refer a patient to Duke Heart or learn more about the Center for Aortic Disease (PDF).
When a thoracoabdominal (TAAA) or paravisceral aortic aneurysm encroaches upon or encompasses visceral vessels, traditional endovascular aneurysm repair (EVAR) cannot exclude the aneurysmal pathology without covering the visceral segment. With limited custom commercial graft availability, open surgery was the only option for patients with this type of challenging anatomy.
Duke Health has established a physician-modified endografts (PMEG) program to customize aortic grafts to the patient’s anatomy, initiated and led by vascular surgeon Chandler Long, MD, co-director of the Duke Center for Aortic Disease. “Few health systems have the infrastructure and skillset to treat complex aortic pathology,” says Long. “Even fewer have the sustained volume to ensure consistent quality outcomes.” Long has also performed this fenestrated-branched EVAR for an aneurysm of the aortic arch, a newer, off-label procedure.
Modifying the endograft
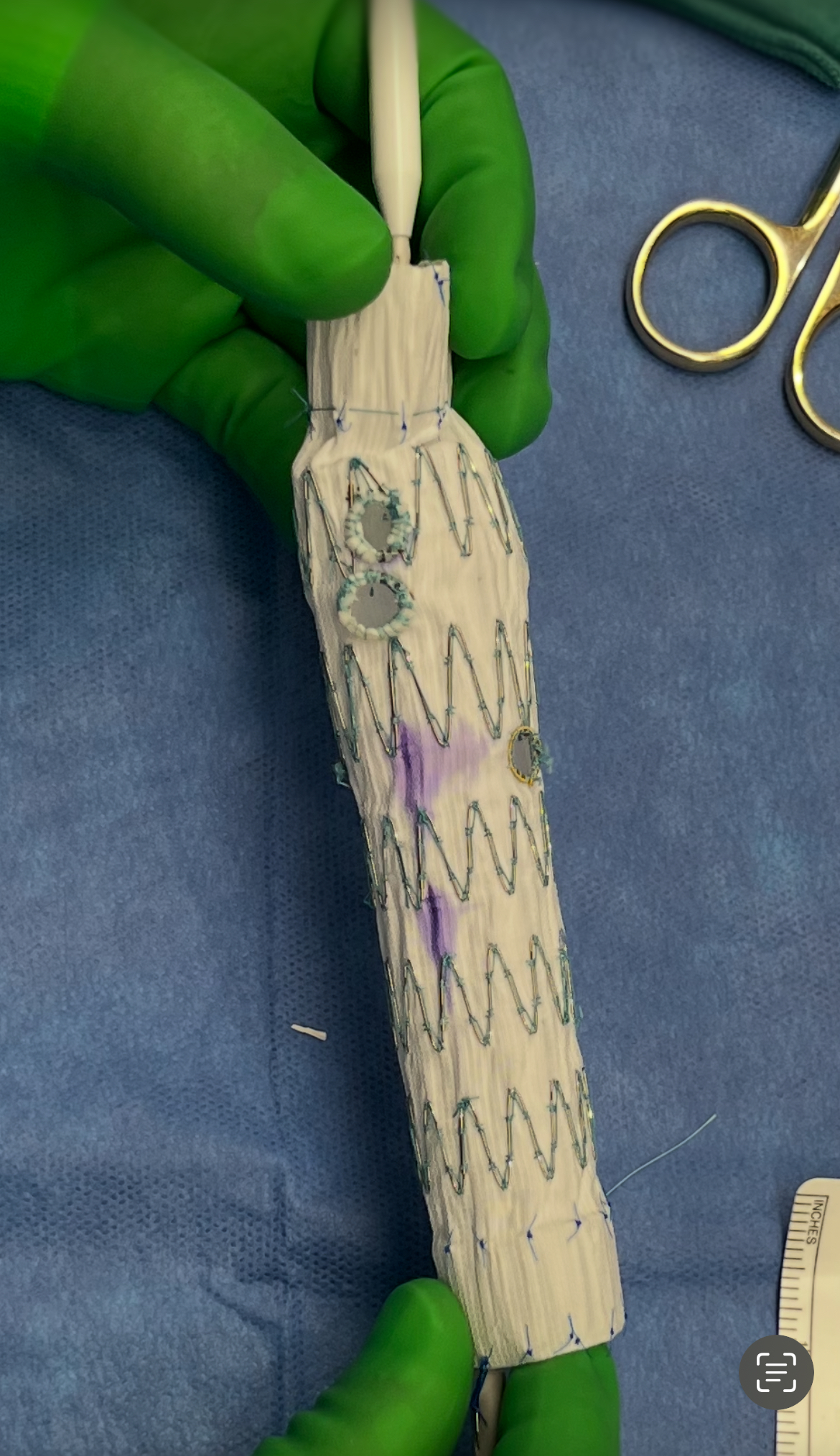
The endograft is modified for each patient individually. Advanced CT imaging software identifies the visceral vessels’ exact longitudinal and radial positions. The surgeon then deploys the graft in a sterile setting and creates corresponding fenestrations with a fine-tip cautery, reinforcing the fenestrations with gold wire for strength and fluoroscopic visibility. If needed, small branches are sewn to the fenestrations for additional support. The graft is then re-constrained, re-sheathed, and placed in its original delivery system.
“Patients with a TAAA that involves the visceral segment could be candidates for this procedure, especially if open surgery poses a prohibitive risk,” says Long. Patients can start surveillance at Duke early on, but any patient with a TAAA with the greatest diameter of at least 5.5 cm should be referred, he adds.
The Aortic Center is strengthening its ability to deliver high‑volume, highly specialized care for referring providers by adding former Duke integrated-cardiothoracic surgery resident Andrew M. Vekstein, MD, to the faculty. “He will be a tremendous force multiplier for our research efforts and is an excellent surgeon,” Long says.
The Duke edge
Long’s research has shown that patients receiving PMEGs have a shorter hospital stay with no significant differences in 30-day or in-hospital mortality, two-year survival, and aorta-specific mortality or reoperation compared to open surgery. This research contributed to the FDA recently awarding Long a physician-sponsored investigational device exemption (PSIDE) for the Duke Customized Aortic Aneurysm Repair With Endovascular Stent-grafts (CARES) Trial.
“We’re one of only a handful of sites in the country to track outcomes from this procedure as part of this FDA-approved clinical trial,” says Long.
Whether patients need open surgery or vascular treatment, the Duke Aortic Center is one of the few centers in the nation with a high level of expertise in both areas to treat aortic pathology, including aneurysms, dissections, and aberrant embryologic anatomy. “Given our collective expertise in aortic surgery, we approach each patient with an individualized plan built with a broad tool belt,” says Long.