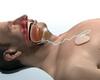
Since 2017, when Duke became the first center in North Carolina to offer hypoglossal nerve stimulator (HGNS) implementation, the demand for this method to treat moderate to severe obstructive sleep apnea (OSA) has increased dramatically. As a Duke otolaryngologist, Russel R. Kahmke, MD, MMCi, FACS says that 50% of his practice has become dedicated to evaluating and treating snoring and obstructive sleep apnea, but there is still a significant population of patients across the country with this condition who are not being treated or do not like their current treatment.
The implanted device (Inspire Medical Systems, Inc.: Minneapolis, MN)—which is often sought out as an alternative to continuous positive airway pressure (CPAP) therapy—works by electrically stimulating the hypoglossal nerve, causing timed tongue movements to relieve upper airway obstruction during sleep. Kahmke notes that while this option is not appropriate for everyone, it has helped more than 50% of his patients achieve an Apnea Hypopnea Index (AHI) score of zero—essentially curing their obstructive sleep apnea—and 97% report seeing some benefit.
In this Q&A, Kahmke explains how this treatment option compares with other surgical interventions, which patients are appropriate to refer for HGNS, and how he sees this technology evolving in the future.
How would you compare the benefits of the HGNS implant and other surgical interventions for obstructive sleep apnea?
Our goal with surgical management of obstructive sleep apnea is to have an AHI reduction of at least 50% with fewer than 20 events per hour of sleep. However, many upper airway surgeries for OSA can be painful to recover from and temporarily impact a patient’s ability to swallow and speak. Unfortunately, in some cases, their condition will regress over time to the point where they’ll begin to experience sleep apnea again. On the other hand, there is increasing data to suggest that the clinical benefit a patient sees immediately after HGNS implantation tends to be the result you get for years to come. The implant is a minimally invasive, same-day outpatient procedure with low downtime and a high potential cure rate. We have been able to achieve surgical success in around 90% of people who are implanted.
How do you measure the effectiveness of the HGNS implant?
Ultimately, our greatest concern from a patient health standpoint is a risk reduction for associated conditions such as stroke, hypertension, and diabetes mellitus type 2, but we also gauge patient satisfaction, tiredness, and global well-being as important metrics. For example, we have plenty of people who feel great and sleep better after they receive the implant, but they still have evidence of apnea; in that case, we’ll do advanced diagnostics and make any necessary changes on the device. If patients continue to experience clinically significant OSA, we can explore other treatment options, both medical and surgical.
Why isn’t this treatment appropriate for everyone?
This technology was designed for patients with moderate to severe obstructive sleep apnea who are not obese and who cannot tolerate CPAP. Sleep is complex, and poor-quality, nonrestorative sleep is more than simply the number of obstructive events per hour. There are many other aspects impacting the quality of a patient’s sleep that should be addressed; being assessed at a high-volume center like our Duke Sleep Disorders Clinic can help patients get linked with the right provider, be that neurology, pulmonology, and psychiatry. If a patient’s BMI is over 40, or if their BMI is over 35 and they have a comorbidity such as heart disease, we get them referred to bariatric surgery or a weight loss management program.
How do you see this technology potentially evolving over time?
The current surgical standard for HGNS implementation is three (or even two) small incisions (i.e., under the jaw line and on the front and side of the chest), but I think advances in the device technology will include standardization to two incisions with even more minimally invasive approaches. Additionally, further iterations of the implant may include cloud-based software for remote device access that will enable us to interrogate and adjust it virtually for patients instead of only on site.