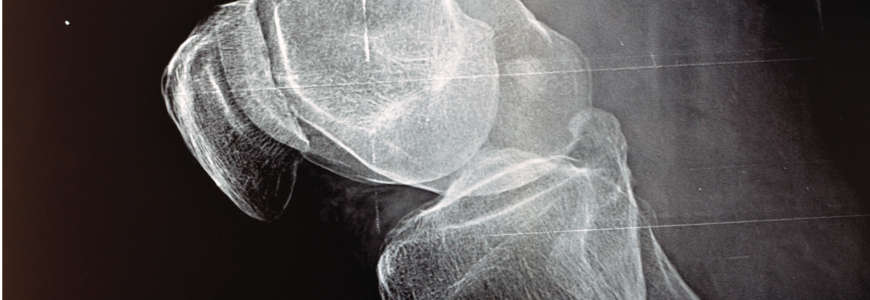
Charcot arthropathy often presents in people with peripheral neuropathy, particularly those who have diabetes mellitus. These patients often present with a red, swollen foot, and their condition prevents them from sensing an injury sustained to the foot. Without proper intervention from an orthopaedic specialist, the ulcer can become infected, the foot can fracture and become deformed, and a leg amputation may be necessary.
“These are very complicated cases, and it can be difficult to know what to do for these patients, so they are often referred too late,” says Samuel B. Adams Jr., MD, a Duke foot and ankle orthopaedic surgeon. “Every case is a little different; it really depends on the characteristics of the foot and the total body.”
Adams notes that patients are often first referred to wound care for the ulcer, but that this can create more problems than it solves. “As soon as the patient starts putting weight on their foot again, the ulcer comes right back because the underlying deformity is still an issue,” Adams explains. “It’s important to not assume it’s just an infection, as it could be Charcot.”
The comprehensive care available at Duke to correct the deformity associated with Charcot arthropathy involves an interdisciplinary team of orthopaedic surgeons, endocrinologists, infectious disease specialists, physical medicine and rehabilitation specialists, and physical therapists. If amputation is needed, the Duke Amputee Clinic will also consult with providers and patients to answer questions and offer guidance about their services.
Adams discusses his general approach for several different types of cases but emphasizes that the treatment plan for each case varies:
- Patient has an infected ulcer: The patient needs to be put in an external fixator for a while, and then return for internal fixation.
- Patient has an impending ulcer: “Our team medically optimizes the patient and performs surgery as soon as we can to change the shape of that foot, and then put the internal fixation in,” he says.
- Patient has uncontrolled diabetes mellitus: To avoid higher complication rates, the patient needs medical management before operating.
To refer a patient, log in to Duke MedLink or call 800-633-3853.
The cases can be technically demanding, requiring up to five hours of reconstructive surgery with multiple experienced OR staff to assist the surgeon. During the surgery, Adams uses a biplanar wedge to cut through their bone, resecting a massive wedge of bone in two planes, which enables him to reconstruct the foot.
“Because patients with diabetes have compromised bone healing ability, I have to ensure that their foot is really physically supported with screws and plates,” he says. “I also want to try to enhance their healing potential by using the biologic stem cells that support bone effusion.”
Although patients can recover from the condition, it can take several surgeries to fully reconstruct the collapsed foot and even more time to rehabilitate. To give them the best chance of healing, Adams keeps patients non-weight bearing for three months, followed by weight bearing and physical therapy.
In addition to his clinical work, Adams leads a section of Duke Orthopaedic Clinician Scientists, a group of Duke orthopaedic surgeons from different orthopaedics subspecialties who are conducting basic science research. (Will Eward, MD, Steve Olson, MD, Julia Visgauss, MD, and Thorsten Seyler, MD, also contribute to this research based on their experience and expertise.)
In his section of research, Adams is investigating the use of a 3D bone block in patients with Charcot arthropathy and has harvested bone from patients with diabetes and healthy patients to determine how well diabetic bone grows onto these 3D implants. “We wouldn’t think it is the same as regular implants, but if it is not the same, we’re looking at what we can do to improve the design so that it can grow into the 3D implants,” he adds.