Duke University Hospital recently became one of the first medical sites in the United States—and the first hospital in North Carolina—with the technology necessary to perform single-port robotic-assisted surgery for partial nephrectomy, a procedure that traditionally requires four to five surgical entry options. This innovative approach is currently FDA-approved for only urologic and ear, nose, and throat surgeries, and is linked to improved patient outcomes and potentially faster recovery times.
Michael N. Ferrandino, MD, a urologic oncologist specializing in robotic-assisted surgical procedures at Duke Cancer Institute, used the new da Vinci SP® Single Port Surgical System (Intuitive Surgical, Sunnyvale, CA) to perform a partial nephrectomy in June 2019 for a patient with small exophytic kidney cancer. As leaders in robotic-assisted surgery, Duke urologists are continuing to study this new technology to identify its potential new role in urologic cancer treatment. In this Q&A, Ferrandino explains this virtually scarless surgical technique through a patient case and its future clinical use.
How is this surgery different from traditional laparoscopic or open procedures for partial nephrectomy?
Ferrandino: This new procedure provides surgeons with robotic-assisted technology that allows us to insert all surgical instruments through one small incision and provides deep access to tissues. We are able to hide a secondary small assisted port incision in the curve of the navel, making it appear to be a scarless surgery.
How is this technique performed?
Ferrandino: The device deploys through a 2.7cm Pfannenstiel incision and enters the abdominal cavity low in the pelvis. After insufflating the abdomen with carbon dioxide and hiding a second incision in the navel as an assisted port, we then attach the robot to the SP trocar that was placed in the initial incision and work from the pelvis up toward the kidney, where we move the intestines out of the way. We identify the renal vasculature and expose the parenchyma of the kidney, thereby identifying the tumor. Using intraoperative ultrasound to ensure that we have identified the lesion correctly and that there are no other lesions in the kidney, we then demarcate the borders of the tumor itself. Next, we place a small bulldog clamp to control the arterial supply to the kidney on the renal artery and surgically excise the tumor. Sutures are placed in the base of the defect to provide hemostasis.
What led you to choose this novel approach for the patient you recently treated?
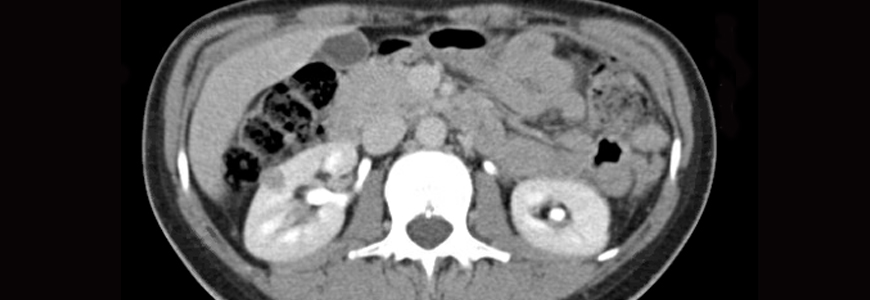
Ferrandino: The first patient to undergo this type of partial nephrectomy was a 35-year-old woman with small exophytic kidney cancer. She was lean and fit when she presented, which gave us more working space, and the lesion was in a good place for the procedure. Especially when using new technologies, we want to minimize any increased risk to optimize patient outcomes up front. Patients who need more extensive, complex surgeries, or who have other compromising issues such as obesity, would not be good initial candidates for this approach while we work our way through the learning curve.
How do patient recovery times compare to traditional methods?
Ferrandino: This technique and technology warrants further exploration and utilization, but so far, reports are that recovery is compatible to, if not slightly improved over standard robotic-assisted surgery, and hospitalization should be about one day. After the surgery in June 2019, my patient spent one night recovering in the hospital before being discharged. She has continued to do well post-operatively and has recovered well. In December 2019, she will undergo a CT scan to confirm the cancer did not metastasize and will visit Duke once a year for routine scans. My hope is that with this new technology, we will be able to improve patient outcomes and have minimal to no impact on overall long-term renal function.
Besides partial nephrectomy, what other surgical applications does this approach have?
Ferrandino: This approach is a step forward with technology and equipment that can be used for pyeloplasty, urethral reimplantation, prostatectomy, partial septectomy, and adrenalectomy. Virtually all surgeries that can be performed laparoscopically and with robotic assistance can use this single-port approach. To date, we have performed partial nephrectomies, prostatectomies, and renal reconstructive surgeries with the SP robot.