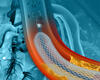
Duke cardiologists performed a novel transcatheter stent procedure for an 80-year-old patient as an alternative to a complex surgery to treat a previously undiagnosed congenital heart condition known as superior sinus venosus atrial septal defect (SVASD).
Duke Adult Congenital Heart Center Director and Interventional Cardiologist Richard A. Krasuski, MD, performed the catheter procedure in collaboration with Gregory A. Fleming, MD, MSCI, a pediatric interventional cardiologist, for the first time at Duke in April 2021. It was the third procedure of its kind in the U.S. The technique was pioneered in Europe by pediatric cardiologist, Sir Shakeel A. Qureshi, MBChB. Dr. Qureshi is based at Evelina Children’s Hospital in London.
The patient initially sought medical care at a regional hospital after experiencing rapidly advancing loss of stamina related to the congenital defect, Krasuski says. The patient’s physicians urged him to be assessed at a center experienced in treating atrial cardiac defects. He then self-referred to Duke Health.
Because of the patient’s age, Krasuski recommended the patient consider the catheter-based option as an alternative to the Warden procedure, the complex, open-chest surgery that has been the standard of care for decades. The transcatheter procedure allows blood to return to the lungs and systemic circulation separately to prevent unnecessary mixing, easing the cardiovascular system workload. Placement of the stent allows blood to flow through or beside the device to restore healthy circulation in the heart, Krasuski explains. At the time of the procedure, approximately 160 catheter-based stent placements had been completed worldwide to correct SVASD.
Krasuski and Fleming researched the procedure extensively, relying on virtual learning during the COVID-19 pandemic. Images related to the patient’s condition were reviewed by Dr. Qureshi and his colleagues; during the procedure, Qureshi and his team participated remotely and provided continual feedback.
Transcatheter SVASD correction gains momentum
Transcatheter correction of SVASD is gaining momentum as cardiologists explore alternatives to the surgical option, particularly for older patients. A 2020 study published in the Journal of the American College of Cardiology reviewed 48 patients who underwent the transcatheter procedure. One of the first studies analyzing SVASD outcomes, the authors concluded that the catheter option is “an attractive alternative” to surgical treatment. They cautioned, however, that 3D reconstruction of cardiac MRI or CT imaging is essential to select patients most likely to benefit. Krasuski used CT and MRI imaging to prepare for the percutaneous procedure.
Originally described in 1858, the condition accounts for approximately 4 to 11% of atrial septal defects. The typical malformation is an interatrial connection caused by a defect in the common wall between the SVC and the right-sided pulmonary veins. An SVASD diagnosis poses multiple challenges because of the wide variety of symptoms as well as the need to select effective imaging to confirm the condition and recommend appropriate therapy.
Krasuski also collaborates with the Duke Center for Pulmonary Vascular Disease to treat patients with chronic thromboembolic pulmonary hypertension (CTEPH). In 2018, he introduced another therapy at Duke--balloon angioplasty (BPA), a catheter-based alternative to pulmonary thromboendarterectomy (PTE), the surgery commonly required for patients with CTEPH. BPA opens vessels and improves blood flow to promote healing of diseased tissues that encourages vascular remodeling. Krasuski has now performed more than 100 BPA cases.
To arrange an assessment for SVASD or any other congenital cardiac condition, contact the Duke Adult Congenital Heart Disease Service at 919-681-3763.
SVASD: A rare and challenging congenital heart condition
Sinus venosus atrial septal defect (SVASD) allows shunting of blood from systemic to pulmonary circulation, but for decades, the standard of care has been the Warden procedure, a complex, open-chest surgery.
The condition—originally described in 1858—accounts for approximately 4% to 11% of atrial septal defects. The typical malformation is an interatrial connection caused by a defect in the common wall between the SVC and the right-sided pulmonary veins. The diagnosis poses multiple challenges because of the wide variety of symptoms, as well as the need to select effective imaging to confirm the condition and recommend appropriate therapy.