New Drugs Raise Hopes for Patients With Sjögren Syndrome
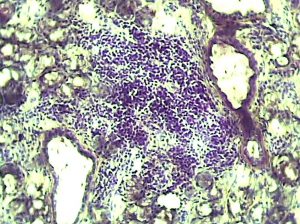
Historically, patients with primary Sjögren syndrome have had few effective, biologic options, but ongoing clinical trials may offer promising new options.
Worldwide, several drugs are being tested in small, randomized trials in the hopes that they may produce targeted treatment for specific manifestations of the disease. The Table below provides a snapshot of several promising clinical trials. It is not intended as a complete list of drugs in development to treat primary Sjögren syndrome.
An incomplete understanding of disease pathogenesis has hampered drug development for this syndrome, says William St. Clair, MD, chief of Duke's Division of Rheumatology and Immunology. A clinician and researcher, St. Clair works regularly with patients who have Sjögren syndrome and investigates new treatment options.
"We face significant, unmet therapeutic needs with Sjögren syndrome," St. Clair says. "Our treatment approach is limited to symptomatic measures. What is missing is an approved, truly disease-modifying drug."
A somewhat rare disease, the condition occurs in 0.2% to 1.4% of the population, affecting about 1 million to 2 million people in the United States. The disease typically presents between 40 and 60 years of age and affects women more than men in a 9-to-1 ratio.
Symptoms include tear and salivary gland involvement, resulting in dry eyes and dry mouth. Extraglandular manifestations may target the joints, skin, kidneys, central nervous system, and lungs.
Although they are small in scope, trials of select novel formulations have attracted attention from clinicians, St. Clair says. Previous trials of anti–tumor necrosis factor α therapies (infliximab, etanercept), for example, showed no improvement in tear and salivary flow, leading to initial disappointment among researchers. Several new, potentially disease-modifying drugs in the pipeline have renewed clinical optimism.
St. Clair says existing treatment options include sialagogues such as pilocarpine and cevimeline that are approved by the US Food and Drug Administration for the treatment of glandular manifestations of Sjögren syndrome. Medications used to manage systemic conditions—prednisone, hydroxychloroquine, methotrexate, azathioprine, mycophenolate mofetil, and cyclophosphamide—are used empirically on a case-by-case basis.
Rituximab may be considered as an option for select adults with systemic disease conditions such as vasculitis, severe parotid swelling, inflammatory arthritis, pulmonary disease, and severe neuropathy. However, 2 randomized, placebo-controlled clinical trials failed to demonstrate the clinical effectiveness of rituximab therapy in those with primary Sjögren syndrome.
"These results may not tell the whole story," says St. Clair. "At this point, we just do not have the biologic therapies we need to manage this disease. We are hopeful the new approaches will produce results."
Table. Select Drugs Being Studied for Use in Sjögren Syndrome
| Formulation | Clinical Trial Number |
| Abatacept | NCT02915159 NCT02067910 |
| AMG 557 | NCT02334306 |
| Belimumab/rituximab vs belimumab | NCT02631538 |
| CFZ533 | NCT02291029 |
| Low-dose interleukin 2 | NCT02464319 |
| Tocilizumab | NCT01782235 |
| UCB5857 | NCT02610543 |
| VAY736 | NCT02149420 NCT02962895 |

