Treatment Alternatives in Charcot Arthropathy of the Foot
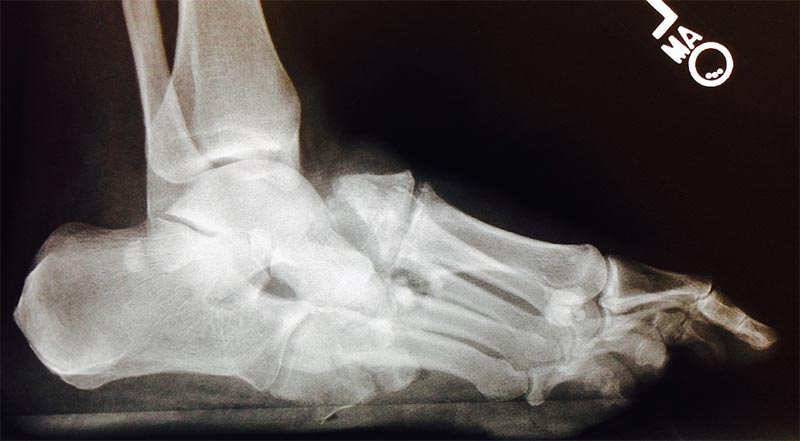
FIGURE 1. Progressive fragmentation and collapse 2 months after initial presentation
A 72-year-old man with type 2 diabetes mellitus was referred to Duke Medicine in October 2014 for treatment of Charcot arthropathy of the foot, a sequela of diabetes. Although his blood glucose levels had been well controlled for 5 to 6 years, he developed numbness, pain, and peripheral neuropathy in both feet.
“Charcot arthropathy is an uncommon complication in patients with longstanding diabetes and peripheral neuropathy," says Beatrice Hong, MD, a diabetologist at Duke, who did not treat the patient. "The presentation is variable, initially with warmth and swelling that progresses into a characteristic collapse of the arch of the midfoot resulting in bony prominences.”
One month earlier, the patient had noticed redness and swelling in his left foot. He received treatment for presumptive cellulitis. Radiographs were obtained at that time, but the initial Charcot fragmentation went unnoticed. He was discharged home on oral antibiotics and his symptoms appeared to improve.
However, at the end of September, he experienced a collapsing sensation of the arch of the affected foot. He continued to bear weight and walk on the foot, and he developed a skin ulcer on the lateral plantar aspect. He sought medical care again and was treated with local debridement and more antibiotics.
In October 2014, he was referred to a local orthopaedic surgeon who diagnosed Charcot arthropathy of the midfoot based on radiographic findings (Figure 1). Due to severe arthropathy, osteomyelitis, and skin ulceration, the patient was offered below-the-knee amputation or referral for a second opinion at Duke.
Question: What are the treatment alternatives for Charcot arthropathy of the foot and can amputation in this case be avoided?
Answer: If it is diagnosed before destructive changes of the bone/joint take place, Charcot arthropathy can often be managed with casting, offloading braces, custom shoes, and orthotic devices. However, when the bones and joints have become unstable, fragmented, and malaligned with compromised skin and soft tissue, surgery is typically necessary. Reconstructive surgery might work as an option to avoid amputation.
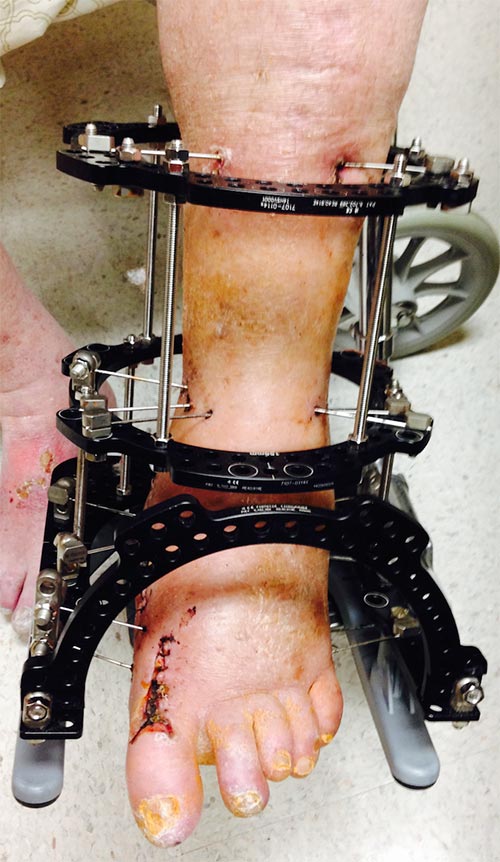
FIGURE 2. Patient's foot positioned in the Ilizarov frame 3 weeks after surgery
In Charcot arthropathy of the foot, the goal of surgical intervention is to realign and stabilize the foot with osteotomies, arthrodesis, and internal and/or external fixation. Unfortunately, the foot cannot always be salvaged, and amputation may be necessary for some patients.
Many factors influence patient outcomes, including loss of protective sensation in the lower extremities, obesity, poor bone and soft-tissue quality, peripheral arterial disease, and immunosuppression.
At Duke Orthopaedics, the patient met with foot and ankle specialist Karl Schweitzer Jr, MD, to discuss possible treatment options.
“In a normal foot, the innervation to the joints keep us from putting too much pressure on our feet, but, in patients with peripheral neuropathy, that protective sensation is diminished or absent,” he explains.
This particular patient was in the fragmentation/dissolution stage of Charcot arthropathy. “Many of these folks get missed, because, clinically, it looks like an infection and x-rays are not obtained or considered,” Schweitzer surmises.
Schweitzer offered reconstructive surgery as an alternative to amputation. “I told him that we could try to salvage his foot,” Schweitzer says, but he made no promises. The patient agreed, and the procedure took place in November 2014.
Osteotomies were performed to help realign the patient’s foot and prepare the bone surfaces for fusion. Rather than using internal fixation, which can be a site for infection, Schweitzer applied an Ilizarov frame, a specialized form of external fixation stronger than conventional external fixation systems (Figure 2). Thin metal wires were positioned in the bone at points along the foot, ankle, and lower leg, and then attached to a frame of aluminum rings and stainless steel rods.
Schweitzer explains that the wires are tensioned within the frame. “It is so strong,” he explains, “that we allow the patients to weight bear in the frame.”
The patient wore the apparatus for 3 to 4 months, which is how long it takes to achieve adequate stabilization. However, after 4 to 6 weeks, Schweitzer added a rocker attachment on the bottom of the frame so the patient could walk on it, thus gaining some mobility and independence.
At 3.5 months, computed tomography revealed that the foot had healed and no residual osteomyelitis was present. Schweitzer removed the frame and transitioned the patient to a fracture boot and then finally to a custom diabetic shoe.
“Now he’s infection free, ulcer free, and, more importantly, he still has his foot,” Schweitzer adds.
Schweitzer stresses the importance of a multidisciplinary approach with these patients. “The surgery itself is only 1 component. It takes infectious disease and hospitalist medicine specialists, along with physical therapy, nursing, and nutrition services, to appropriately care for these patients,” Schweitzer explains.
He also emphasizes that Charcot arthropathy is commonly misdiagnosed early on as soft-tissue infection or cellulitis, as was the case with this patient. So, he elucidates, primary care providers and emergency department physicians should maintain a high index of suspicion for Charcot arthropathy in patients with diabetes who have redness, swelling, pain in the foot, or a combination of all 3 symptoms.