Treating Spontaneous Foot Weakness Causing Immobility
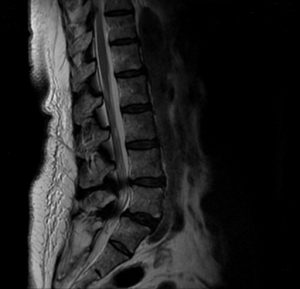
FIGURE 1. Sagittal magnetic resonance
imaging obtained preoperatively shows spondylolisthesis at L5/S1 and stenosis at L4/5 and L5/S1
A 69-year-old woman presented at Duke with weakness in both feet that caused her to be unable to walk without the use of an ambulation device.
The patient explained that, 2 weeks prior, she had been in a crouching position when she stood up and spontaneously experienced weakness in both feet and her toes. She was not experiencing pain.
After 2 visits to the emergency department, being hospitalized for several days, and undergoing magnetic resonance imaging, the patient had not received a diagnosis or treatment. Frustrated and concerned about what the symptoms meant for her mobility, she was referred to Duke and orthopaedic spine surgeon Norah Foster, MD.
A review of the earlier findings on magnetic resonance imaging of the patient’s lower spine revealed stenosis, which was likely causing the weakness in her feet. Radiography was obtained and revealed arthritis in the lumbosacral joint (L5-S1) and spondylolisthesis at the L4-L5 spinal segment (Figure 1). A brief, 5-day course of steroids provided the patient no benefit.
Question: How did Foster restore feeling and mobility in the patient’s feet?
Answer: The patient underwent surgery to posteriorly decompress the spine from L4 to S1 and a transforaminal lumbar interbody fusion at the L4-L5 and L5-S1 levels. Foster also conducted a posterior instrumented fusion of the patient’s spine, placing screws and rods at the L4, L5, and S1 pedicles.
The patient regained feeling and movement in her feet immediately following surgery. Six weeks postoperatively, she had regained full strength in both feet and was experiencing no postoperative pain. She was able to walk without braces and relied on an ambulatory device only for long distances. After being unable to work for months, the patient was on track to return to her job approximately 12 weeks following surgery.
“My goal was to relieve the pressure on her nerves so that they would function again. But I had to explain to her that the outcome was not guaranteed,” says Foster. “Approximately two-thirds of patients will experience improvement after surgery, but they won’t necessarily be back to ‘normal’ again. The other one-third won’t see any benefit at all. Unfortunately, we don’t know what the outcome will be until the surgery is performed, so you have to hope for the best.”
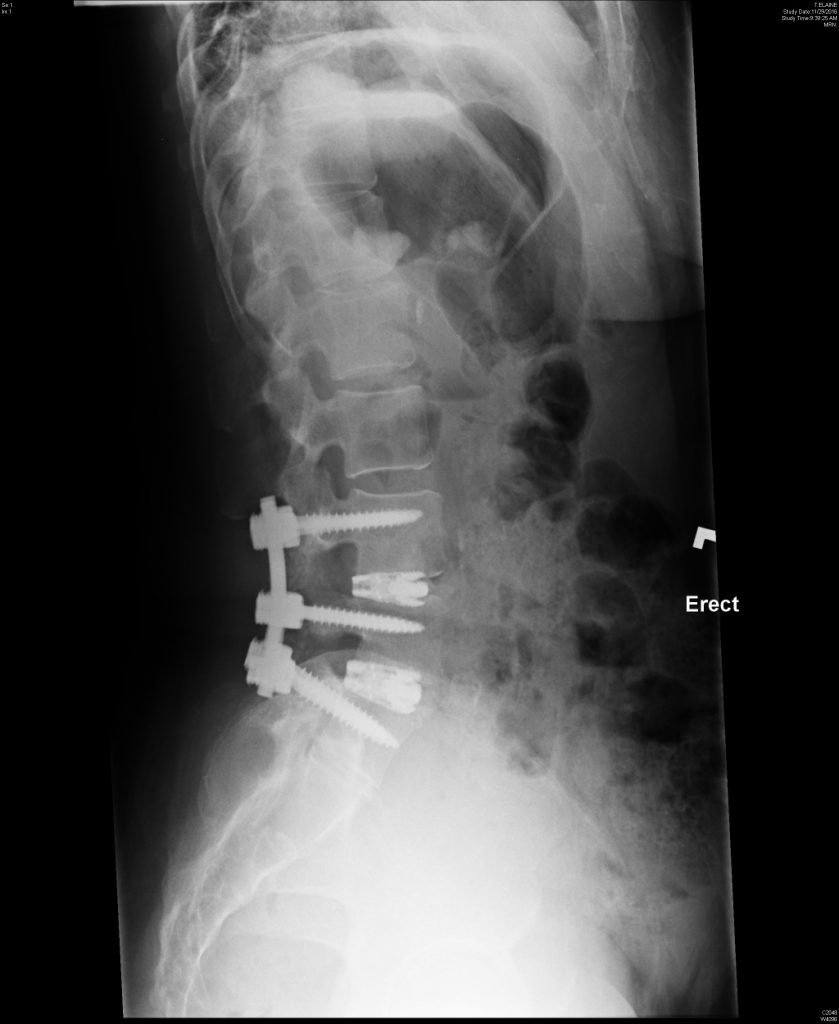
FIGURE 2. Radiography obtained 6 weeks postoperatively showing the hardware in a good position and reduced spondylolisthesis
Radiography obtained postoperatively during follow-up appointments indicated progress and that “the hardware looks good,” says Foster (Figure 2).
“She was the ideal patient because she listened to medical advice and maintained a positive outlook, despite not knowing the outcome,” continues Foster.
“We discussed and managed her expectations, but it would have been easy to be negative. She went from being an independent person to requiring assistance for day-to-day activities. Now, she’s back to normal and can walk without a walker.”