A new Duke research study will use computational fluid dynamics (CFD) methods to analyze the severity of unilateral cleft-induced nasal dysfunction and size of obstructed sites, assess the impact of current treatment modalities in restoring function, and identify the surgical procedures that will optimize patient outcomes. This study will be the first of its kind to specifically target cleft-induced nasal dysfunction for development of treatment options that will optimize surgical outcomes using virtual surgery and CFD modeling.
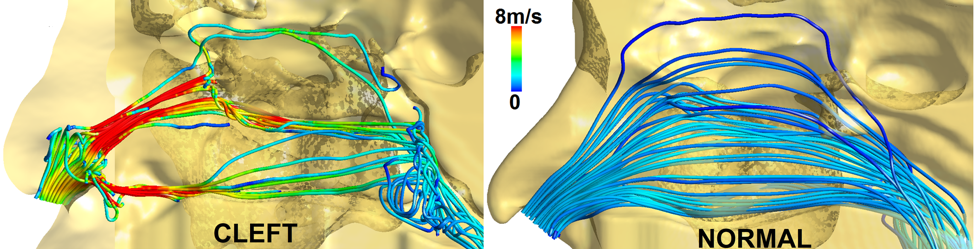
“Much progress has been made in restoring ‘form’—the external, aesthetic aspects of the deformity—but not much work has been done on restoring ‘function’—the internal nasal deformity that results in difficulty breathing and impacts quality of life,” says Dennis Onyeka Frank-Ito, PhD, assistant professor of surgery at Duke and lead investigator for the study. The study is funded by a grant from the National Institute of Dental & Craniofacial Research of the National Institutes of Health under Award Number R01DE028554 and will enroll 30 patients.
“An estimated 70% of individuals with unilateral cleft-induced nasal deformity have impaired nasal function,” Frank-Ito says. “When these patients are asked about their nasal function, they often underreport the severity of their symptoms because the emphasis has been on how they look, and they’ve never experienced normal nasal function so they don’t know what it feels like to breathe normally.”
Frank-Ito explains there are three primary pillars of the study:
- Investigate at a macro level how effective current surgical intervention is in restoring nasal function
- Investigate at a micro level how well current interventions target the most relevant size of nasal obstruction in these patients
- Use CFD methods to determine the surgical type that can optimize patient outcomes
Researchers will use scientific imaging software to create 3-D reconstructions of patients’ airways based on preoperative and postoperative CT scan images, after which computational meshes will be generated to numerically compute airflow in the airway. Researchers will evaluate the surgery that was performed on each patient to determine how well it targeted the most obstructed sites.
These results will then be compared with results from virtual surgery models mimicking different procedure types that could have been performed, enabling researchers to conclude which surgical technique is optimal for each patient. It will also serve as a tool for researchers to make recommendations for the types of surgery that will yield the best patient outcomes with the minimum amount of risk.
Jeffrey R. Marcus, MD, chief of plastic surgery and director of the Duke Cleft and Craniofacial Center, is the lead surgeon and co-investigator for the study. “Among all rhinoplasty operations, the surgery for the cleft nasal deformity is the most challenging and the most complex, both functionally and cosmetically,” says Marcus, who is also immediate past-president of The Rhinoplasty Society. “However, Dennis and I have recognized that the deformity has a consistent pattern in many ways from one person to the next, with certain exceptions. This makes it possible to conceive of a treatment plan that will consistently work.”
Frank-Ito and Marcus encourage cleft surgeons to focus on function as well as appearance. Surgery for the cleft deformity requires knowledge of cleft anatomy, rhinoplasty technique, and nasal function. The dilemma many face is that few surgeons have expertise in all three of these areas. When a surgeon from one particular training background lacks a certain expertise, he/she can identify a colleague who may be able to collectively plan and carry out a comprehensive procedure.