Duke is a leading national referral center for Moyamoya disease and is now one of very few academic medical centers in the world with multiple specialists who have experience caring for children and adults with the condition. Gerald A. Grant, MD, recently returned to Duke from Stanford to serve as chair of the Department of Neurosurgery and adds his Moyamoya expertise in pediatric and young adult cases to that of Ali R. Zomorodi, MD, who specializes in adult cases.
Moyamoya—a chronic, progressive cerebrovascular disease which reduces blood supply to the brain—can cause devastating strokes and seizures for patients if left untreated. It is rare, affecting about one in one million people each year, but may occur at any age. Peak incidence periods are between ages 5-10 in children and ages 30-50 in adults.
Duke’s outcomes and emphasis on the patient and caregiver experience have helped to solidify its reputation as a referral center in the Southeast for confirming diagnoses, consulting on complex cases, and caring for patients who have been turned away elsewhere.
“Nothing we do matters unless we pay attention to the patient experience, starting at the referral process and at every step along the way,” Grant notes. “It’s not enough for a patient to get great care—they must have trust to know that they are getting the best possible team-based care at Duke Neurosurgery.”
Duke specialists can offer access for new patients within 7 days
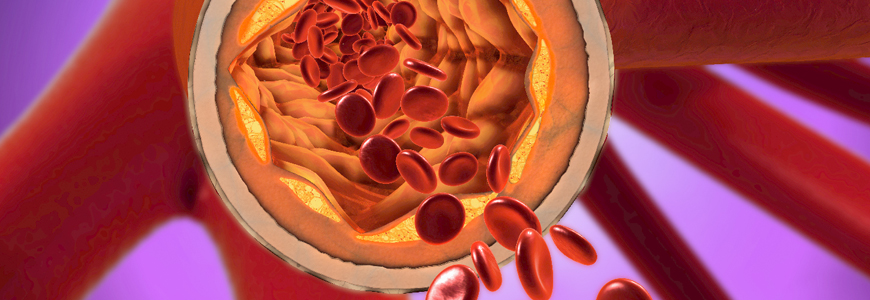
Presenting as occlusion or stenosis of the carotid artery at the skull base, the condition gradually reduces blood flow perfusion to the brain. To compensate for blocked or narrowed arteries, the brain creates collateral vessels to maintain blood flow to the brain. “Because the disease clips off the blood vessels that keep occluding, the blood starts to flow from the outside in, which can cause bleeds, seizures, stroke, or aneurysms,” Grant explains.
Grant and Zomorodi both have experience in treating Moyamoya cases to help relieve symptoms and reduce risk for serious complications. “Through the extraordinary surgical care and patient experience we provide at Duke, we help to ensure that our patients’ chance of future stroke or hemorrhage is as low as possible, and that we maximize their quality of life,” Grant adds.
Duke specialists can offer access for new patients within 7 days and can provide faster access for urgent issues. Patients receive a full workup and advanced imaging studies, which may include magnetic resonance angiography, computed tomography angiography, or cerebral angiography. The surgeon then reviews the case with experts in related disciplines to determine the best course of action for revascularizing the brain.
“It’s important to not rush patients with Moyamoya into a bypass,” Grant says. “After an adverse event, the best thing for a referring provider to do is to let them stabilize, work them up, and then refer them to a center like Duke with experienced neurovascular surgeons who are very familiar with performing these complex types of procedures.”
Although treatment for Moyamoya disease is not usually urgent, it does require a highly complex and time-sensitive cerebral artery bypass to reroute blood flow around the occluded artery. “You’re on the clock because you need to perfuse the brain as soon as possible again after clamping the blood vessels and interrupting the blood supply,” he says. “Because of this, the stroke risk for this procedure is temporarily higher because you need to isolate the donor vessel, usually in front of the ear, and hook it up to one of the brain blood vessels to bypass the blood flow.”
Duke offers a dedicated physician referral to help you and your patients access the care you need by calling our nurse navigator Berrin Ammons at 919-604-3964.
Considerations for treating children with Moyamoya disease
Cerebral artery bypass in young children is used less frequently because of the small caliber of blood vessels, but experienced medical management is essential. In children, Grant says the approach is often to lay the donor vessels on top of the brain surface to improve blood flow to the brain from outside to inside through an encephaloduralarteriosynangiosis (EDAS) procedure.
However, for older children and young adults, Grant notes that collaboration is key to perform a direct bypass. The partnership between the pediatric and adult neurosurgery and stroke neurology teams helps bridge the potential gap in care for these patients, who require lifelong follow-up care.
“Partnering with an adult cerebrovascular surgeon like Dr. Zomorodi, who has an incredible bypass record, is critical to the success of these bypasses in children,” Grant says. The collaboration of perioperative care is also critical to avoiding stroke during and after the surgery, he adds. “It’s so important to know how to assess the anatomy and physiology of patients with Moyamoya disease, individualize their fluid management, and manage their post-operative care.”