Deciding on a Course of Action for a Pancreatic Neoplasm
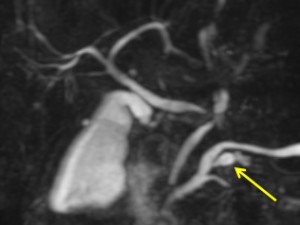
Figure 1. MRCP demonstrating a 9-mm cyst communicating with a side-branch duct in the pancreatic head and mild dilatation of the main pancreatic duct
An otherwise healthy 67-year-old man developed moderate left-sided abdominal pain. An evaluation by his primary care provider revealed that he had elevated amylase and lipase levels consistent with a diagnosis of acute pancreatitis. However, he had no predisposing conditions for pancreatitis, such as gallstones or alcohol misuse.
When patients present with pancreatitis but do not have a history of predisposing conditions, cross-sectional imaging of the pancreas is warranted to rule out neoplasia. Therefore, the patient underwent magnetic resonance cholangiopancreatography (MRCP), which showed a dilated pancreatic duct and a small (9 mm) cyst in the head of the pancreas (Figure 1). Endoscopic ultrasound also revealed mucin emanating from the pancreatic duct orifice, a pathognomonic feature of an intraductal papillary mucinous neoplasm (IPMN).
Question: What would be the best course of treatment for this patient?
Answer: The best course of treatment for this patient was laparoscopic pancreaticoduodenectomy (Whipple procedure).
At this point, the patient was referred to Duke Medicine for further assessment where he saw Rebekah White, MD, a specialist in advanced oncologic and gastrointestinal (GI) surgery.
IPMNs exhibit a wide spectrum of neoplastic transformation ranging from low-grade dysplasia to invasive carcinomas. “All pancreatic cystic lesions should be evaluated by a GI specialist or a surgeon with expertise in this area because it’s hard to know whether these lesions are benign or premalignant,” Dr. White said.
Expert consensus guidelines currently recommend that asymptomatic IPMNs less than 10 mm be managed by observation alone, as these cysts are rarely malignant. However, symptomatic IPMNs and those with features that suggest malignancy (eg, main pancreatic duct dilation of more than 5 mm, larger cyst size, thickened cystic walls, the presence of solid lesions, lymphadenopathy) are best managed by resection. “Even though the cyst was small, we recommended resection based on the symptoms and the dilated pancreatic duct,” Dr. White explained. “Those are things that can be risk factors for malignancy.”
Dr. White recommended laparoscopic pancreaticoduodenectomy (Whipple procedure). The patient agreed to the procedure, which was performed by Dr. White and Duke Medicine GI surgeon Alexander Perez, MD. The postsurgical course was uncomplicated, and the patient was discharged from the hospital on day 7.
Historically, Whipple procedures have been associated with 10% to 15% mortality and high morbidity rates. However, with current techniques, mortality rates at Duke Medicine are less than 5%. Although pancreatic anastomotic leak and delayed gastric emptying are still potential complications, this patient had no difficulties and was back to normal activity in less than 8 weeks.
Pathology revealed a benign side-branch IPMN, but Dr. White sees the patient annually for follow-up because patients with IPMNs have an increased risk of developing other IPMNs and may also have an increased risk of other malignancies. “These patients need life-long surveillance,” Dr. White said, adding that the patient's results on follow-up MRI have been normal, thus far. "His prognosis is excellent, and he can expect to have a normal life expectancy.”
Dr. White commented that the alternative option in this case would have been observation, typically with computed tomography or MRI every 3 to 6 months for newly diagnosed lesions, then every 6 to 12 months after stability is confirmed. However, this patient’s IPMN probably would have caused recurrent episodes of pancreatitis and, eventually, would likely have become malignant.
This highlights the important point that it's often difficult to determine whether IPMNs should be managed with resection or observation alone. For this reason, all pancreatic cysts warrant evaluation by an expert. “Whether to intervene in older patients is an important issue, as it may take 10 to 20 years for an IPMN to become malignant,” she emphasized. “In some patients, resection is not indicated because the patients are more likely to die from other conditions.”