Complex Congenital Heart Condition
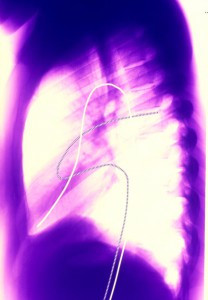
A 32-year-old woman with repaired Tetralogy of Fallot, who recently collapsed after briskly ascending a flight of stairs, came to Duke University Medical Center for a second opinion regarding her management.
She had been seen at a local hospital, where the workup (which included computed tomography to rule out pulmonary embolism, echocardiography to exclude valvular stenosis, and a stress test to rule out coronary ischemia) had failed to demonstrate a clear cause, and she was discharged home.
As a child, the patient underwent a palliative shunt procedure in 1983 and then a complete repair, including patch repair of the ventricular septal defect and resection of the subpulmonic obstruction, in 1987. The latter required the use of a fairly large outflow tract patch. As a result, she developed significant regurgitation of the pulmonic valve.
As a teenager, she also experienced minor rhythm disturbances that were corrected following an ablation procedure. She had been doing well for many years, other than occasional palpitations.
Question: Should additional testing be performed?
Answer: Yes, further evaluation was warranted in this case.
Duke cardiologists found the patient’s story concerning and suspected the patient may have inducible ventricular arrhythmia. Richard A. Krasuski, MD, a professor of medicine and pediatrics and the director of the Adult Congenital Heart Disease Program at Duke University Medical Center, performed cardiac magnetic resonance imaging, which showed severe regurgitation of her pulmonic valve and a significantly enlarged right ventricle. Three-dimensional reconstructions of the imaging showed that the right ventricular outflow tract was very large.
“In such patients, we always look to see whether we can offer a catheter-based intervention. In about one-half of the patients, we can,” Krasuski says. “In her case, however, the outflow tract was too large to place a stent and then implant a transcatheter valve. In addition, there was a large shelf of calcium adjacent to the patch that we felt would be better off resected in the operating room.”
The patient subsequently underwent diagnostic heart catheterization and an electrophysiological study. Because she was fearful of undergoing these procedures, her health care team performed them in a single setting under general anesthesia with an interventional cardiologist and an electrophysiologist working together.
Catheterization showed the expected pressure differences in her right heart and no abnormalities in her coronary artery courses. The electrophysiological study revealed inducible ventricular arrhythmia, just as the Duke team had suspected.
“We believe that the severe regurgitation of her pulmonic valve led to structural changes of her right heart and resulted in arrhythmia and an episode of sudden death,” explains Krasuski. “She needed the valve issue resolved and steps taken to protect her from the risk of future arrhythmias.”
Consequently, a congenital heart surgeon performed open-heart surgery to resect the patch and the significant amount of scar tissue adjacent to it in her right ventricular outflow tract and then implanted a new valve. Following the surgery, a defibrillator was implanted.
This case illustrates Duke’s multifaceted approach to adults presenting with complex congenital heart defects—an approach that Krasuski says was integral to expediting care in this challenging case. “Even though she had complex physiology, we managed it like a routine problem because of our ability to work well as a team,” he says. “The 3 of us quickly and openly communicated about her case, which resulted in the right decision ultimately being made.”
All of the procedures were performed within days at the hospital, and the patient was not required to return repeatedly for care. This fact was important because she was a young mother who lived several hours away. One week after discharge, the patient stopped all pain medications, was starting to regularly exercise, and was doing very well at home.