Clinic Offers Multidisciplinary Care for Rare Rheumatic Disease
A fast-growing Duke Health clinic offers multidisciplinary care for patients with scleroderma by bringing together experienced specialists to treat this rare and challenging disease.
During the course of a few days, a patient can see an expert in scleroderma as well as a pulmonologist, gastroenterologist, dermatologist, physical therapist, and other clinicians who understand the highly variable symptoms of localized or systemic scleroderma.
“Often patients seek our center because their local rheumatology practice does not feel comfortable managing this disease,” says Ankoor Shah, MD, the clinic director.
Many rheumatoid arthritis groups refer patients directly to Duke because of its growing expertise in treating scleroderma. Patients with this autoimmune disorder also tend to be savvy about new treatments, so many find out about the Duke Health clinic’s emerging expertise through personal research.
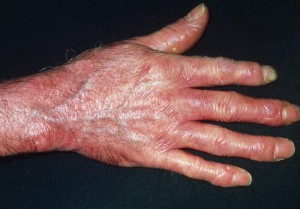
As their skin, organs, and blood vessels may begin to thicken due to the excessive absorption of collagen that characterizes their condition, patients with scleroderma can face unusual and varied symptoms.
“It’s a rare disease and a challenging one,” Shah adds. “A typical rheumatology practice might treat no more than 2 or 3 patients, whereas I’m longitudinally following 70 patients who have many needs.”
The clinic began specializing in scleroderma 2 years ago when Shah asked that all patients be directed toward the collaborative group of clinicians focused on autoimmune disorders.
Using the secure Research Electronic Data Capture database tools popular for research at Duke Health and other leading medical centers, Shah launched a disease registry to monitor scleroderma among its patients.
An orphan disease, scleroderma is often neglected in research because of lacking commercial interest. Shah says the Duke Health clinic uses its growing patient load and database to contribute to the search for a cause and a cure.
The disease affects about 20 patients for every 1 million people, so case numbers are low. The disease disproportionally affects women—particularly younger women. The symptoms can be more severe in men, but not always.
The clinic also plans clinical trials to study the effects of pulmonary fibrosis and hypertension on scleroderma. “Our goal is to identify and leverage translational research to uncover new approaches and put them to use as soon as possible,” Shah says.
Additional research is underway at Duke Health to assess the potential of cellular therapies such as bone marrow transplantation as possible therapy for severe scleroderma, although these approaches have not yet been approved by the US Food and Drug Administration.