Advances in OCT
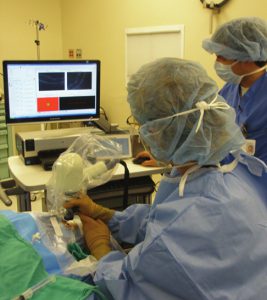
FIGURE 1: Handheld OCT probe held over the patient’s eye during surgery. Reprinted with permission from Carrasco-Zevallos OM, et al. Invest Ophthalmol Vis Sci. 2016;57:OCT37-50.
In the early 1990s, optical coherence tomography (OCT) emerged as a revolutionary new technology in the field of ophthalmology. Representing the first major advance in retinal imaging for almost 150 years, OCT allowed physicians to see beneath the surface of the retina for the first time.
Duke retinal surgeon Cynthia Toth, MD, and her longtime collaborator, Duke professor of engineering Joseph Izatt, PhD, have been at the forefront of OCT innovation virtually since its inception, helping it grow from an idea to the standard of care for adult patients.
Now, with support from the Duke Clinical and Translational Science Institute (CTSI), they are developing a suite of devices and techniques that take OCT out of specialized clinics, allowing it to be used at a patient’s bedside—or even in surgery—to give physicians an unprecedented level of real-time information.
Window to the Brain
“What we at Duke are known for in the OCT world is pioneering the use of handheld probes for pediatric imaging,” says Izatt.
In 2012, a handheld device developed by Toth and Izatt was approved by the FDA for use in humans. The device was taken to market, and, for the first time, there was a commercial alternative to the conventional OCT system—a bulky tabletop setup typically located in an eye clinic’s photography suite and operated by a technician.
While the conventional system requires that the patient be able to follow instructions, such as opening and closing their eyes, looking in different directions, and keeping still, Toth and Izatt’s handheld probe can be used to examine infants and other patients who are unable to respond to instructions such as those under anesthesia. This can provide critical, time-sensitive health information that goes beyond the eyes themselves.
“The retina is an extension of the brain, so it’s a window in,” says Toth. OCT images can reveal neurologic markers that correspond to conditions affecting the brain and help physicians assess whether a treatment is working.
Going 3-Dimensional (3-D)
Five years after their handheld probe was approved for use in humans, Toth and Izatt have continued to expand the frontiers of OCT.
In 2016, they began testing an improved probe that puts powerful new functionality into a more compact, easy-to-use form. Whereas the previous device only did cross-sections, the new device provides full-volume, 3-D images. “It’s smaller, it’s lighter, and it’s faster,” Toth says. “So I can do non-dilated examination and get images through the pupil. One of the things we watch is how the pupils respond, so I can’t use the dilating drops. This system was designed to allow us to do that.”
The ability to do 3-D imaging also opens OCT to a new arena—the operating room. “My dream has been to be able to use OCT pictures in surgery,” Toth says.
With 3-D, surgeons aren’t restricted to a surface or cross-sectional view—they can adjust the image in any direction to interactively monitor the retina as they operate. Toth explains: “It becomes image-guided surgery, and you’re actually watching it dynamically as it’s changing. With OCT, I can see and respond as the tissue moves.”
Toth and Izatt’s inter-surgical OCT research system at Duke is the only one in the world. They are continuing to hone the technology and establish best practices for its use. Ultimately, they envision making the full suite of OCT tools more user friendly.
In the meantime, they are continuing to search for the next revolutionary idea.
“Working at a university and with CTSI is so exciting, because we can brainstorm with smart people across the university and come up with what we think we should be doing next,” Toth says. “I don’t want to just focus on one idea or technology—I like looking forward to the next idea and the next technology.”