Advances in Metabolic Imaging for the Treatment of Head and Neck Cancer
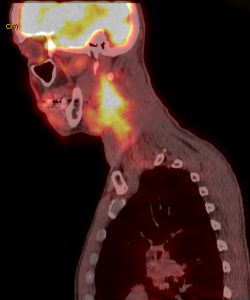
Positron emission tomography (PET) and computed tomography (CT) scans are frequently used to diagnose a variety of cancers, including head and neck cancer. In particular, the imaging techniques are used to detect tumors in the mouth, throat, larynx, sinuses, lymph nodes, salivary glands, and thyroid gland. Duke oncologists are combining PET and CT scans to better diagnose cancers, predict the outcome of a planned course of treatment, and, eventually, personalize treatment strategies for head and neck cancers.
Because CT scans show anatomy and PET scans show activity, combining the 2 scans for fused PET/CT imaging shows both, better informing physicians as to the best course of treatment. Walter Lee, MD, MHS, a head and neck surgeon and co-director of the Head and Neck Cancer Program at the Duke Cancer Institute, explains: “A CT scan will show a mass, and the PET scan will show metabolic activity. Relying on a negative CT scan alone could lead us to think there’s no cancer in a normal-sized lymph node, but a PET scan could indicate the node is metabolically active, thus helping to better direct our diagnosis and treatment for the patient.”
Metabolic imaging is also being used for patients who have undergone surgery and received postoperative chemoradiation therapy but have a high risk of cancer recurrence. If findings on a PET scan are negative after 3 months of treatment, physicians can be confident that the patient has had a complete and durable response; if the scan shows signs of persistent activity, clinicians can develop a new course of action to quickly determine whether it is due to treatment side effects or persistent cancer.
Looking at future advances in the use of metabolic imaging, Lee notes that Duke physicians are currently investigating how PET scans can help clinicians model and personalize treatment during the early stages of cancer. “Radiation treatments are typically 6 to 7 weeks long, but if we can perform a repeat PET scan after just 1 to 2 weeks, it could inform us very early to modify treatment plans based on the tumor’s response.”
Another advantage for patients is the Duke Cancer Institute’s multidisciplinary tumor board, comprising a team of experts that include surgeons, medical and radiation oncologists, neuroradiologists, and pathologists. As a team, they review the patient’s history, including images. “When patients are referred to Duke, they have a whole team of dedicated specialists and a whole package of advanced treatments standing behind them,” says Lee.